Corneal Disorders
26 January 2026 2026-02-16 11:30Corneal Disorders
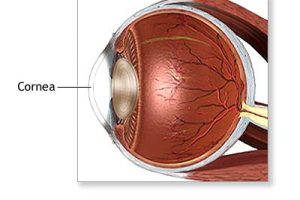
Corneal Anatomy
The cornea is the transparent front part of the eye that covers the iris, pupil, and anterior chamber. Together with the lens, the cornea refracts light, accounting for approximately two-thirds of the eye's total optical power. In humans, the refractive power of the cornea is approximately 43 dioptres.
The cornea has unmyelinated nerve endings sensitive to touch, temperature and chemicals; a touch of the cornea causes an involuntary reflex to close the eyelid. Because transparency is of prime importance the cornea does not have blood vessels; it receives nutrients via diffusion from the tear fluid at the outside and the aqueous humour at the inside and also from neurotrophins supplied by nerve fibres that innervate it. In humans, the cornea has a diameter of about 11.5 mm and a thickness of 500-600 μm in the center and 600–800 μm at the periphery. Transparency, avascularity, the presence of immature resident immune cells, and immunologic privilege makes the cornea a very special tissue.
Corneal Layers:
- Corneal epithelium
- Bowman’s layer
- Corneal stroma
- Descemet’s membrane
- Corneal endothelium
Various refractive eye surgery techniques change the shape of the cornea in order to reduce the need for corrective lenses or otherwise improve the refractive state of the eye.
Orthokeratology is a method using specialized hard or rigid gas-permeable contact lenses to transiently reshape the cornea in order to improve the refractive state of the eye or reduce the need for eyeglasses and contact lenses.
Hellenic Keratoconus Center
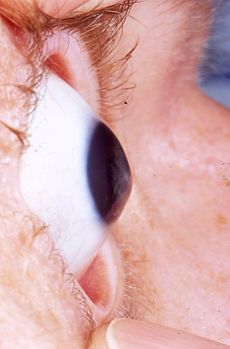
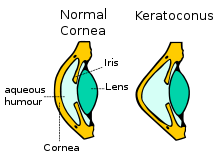
Keratoconus
Keratoconus is a condition of the cornea that appears during adolescence and usually progresses until the fourth decade of life. It typically affects both eyes at different rates of progression. In keratoconus, the central part of the cornea thins and takes on a conical shape instead of the usual somewhat spherical shape. The patient’s vision is blurred due to significant myopia and irregular astigmatism. When it first appears, it can be successfully treated with a regular pair of glasses or contact lenses, but as it progresses, satisfactory vision can only be achieved with the use of specialized contact lenses. In advanced stages, surgery is required.
The LVO is a center of reference and study for this condition, given that corneal transplants in keratoconus were the main research topic of the doctoral thesis (1976-1981) of the former Director of the LVO, Prof. I. Pallikaris, and one of the key factors that contributed to its creation and establishment by him in 1989, the Vardinoyannis Laboratory of Eye Transplantation and Microsurgery.
Today, the LVO conducts studies on the epidemiology of the disease in Greece, as well as on its genetic background, in collaboration with major universities abroad. At the same time, the LVO is at the forefront of global research into the discovery and adoption of the most modern methods for delaying or halting the progression of the disease, improving patients’ visual acuity (vision), and applying minimally invasive treatments for keratoconus, such as corneal collagen cross-linking and the application of intracorneal rings (Intacs). The LVO is one of the first centers to implement these treatments, having operated on one of the largest numbers of patients worldwide, while applying personalized treatment to each patient. The spectacular results of these applications have been published in peer-reviewed international medical journals (these publications are from the largest series of patients with keratoconus, source: http://www.pubmed.org), thus contributing to the further development of these methods.
CXL: Corneal Collagen Cross Linking
A new therapeutic approach for the treatment of keratoconus is the interconnection of the corneal collagen (Corneal Cross Linking, CXL) with the use of riboflavin (vitamin B2) and Ultraviolet irradiation A. The aim is the improvement of the resistance and rigidity of the cornea -stiffening effect- that ceases the development of keratoconus. IVO in this moment is concerned as the world’s avant-garde in the application of this treatment and constitutes a point of reference in CXL treatment.
A one-time application of riboflavin solution is administered to the eye and is activated by illumination with UV-A light for approximately 30 minutes. The riboflavin causes new bonds to form across adjacent collagen strands in the stromal layer of the cornea, which recovers and preserves some of the cornea’s mechanical strength. The corneal epithelial layer is generally removed in order to increase penetration of the riboflavin into the stroma.The duration of the treatment is one hour and it is painless due to the use of local anesthaetic drops. In the end of the treatment, a bandage contact lens is placed in the eye which remains from 4 to 6 days.

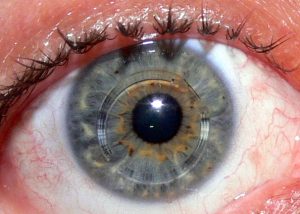
INTACS
The INTACS (Intrastromal Corneal Ring Segments or Intracorneal rings) are small rings of biocompatible material, which are placed in the cornea of the patients with keratoconus in order to improve the topographic images and the visual acuity of the patients.
The placement of the rings demands the creation of a tunnel in the cornea with the use of a 5th generation Laser the iFS Advanced Femtosecond Laser and the patient does not feel them in his eye at all. The placement of Intacs is decided by the surgeon depending on the particular characteristics of each patient. The intervention is conducted under anesthaetic drops and is painless.

Lamellar and Penetrating Keratoplasty
Lamellar and Penetrating keratoplasties are interventions in which total or partial transplantation of the corneal tissue is effectuated for the treatment of various diseases of the cornea that considerably decrease visual acuity.
Keratoplasty can be penetrating (full corneal transplantation) or partial, such as lamellar keratoplasty or endothelium transplantation (DSAEK). Until recently, incisions were made by the use of specially designed surgical instruments which resulted in the need of stitches and high postoperative astigmatism. At LVO those incisions can be performed with the use of the Femtosecond Laser offering numerous advantages. Firstly, we can precisely create the same dimension implant in both donor and recipient corneas and moreover we can give various different shapes. The result is fewer stitches, less post operative astigmatism and graft form depending on our patients needs.
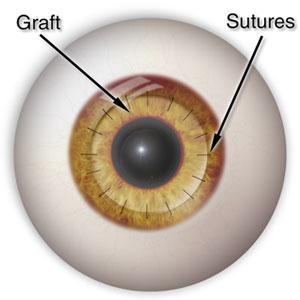
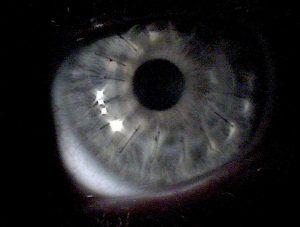
At IVO as well as at the University Hospital Ophthalmology department, apart from the common keratoplasty methods, partial anterior and posterior keratoplasty are performed. These modern applications have good results in respect to the conventional keratoplasty because keratoconus, trauma, corneal scars and enthodethium pathology can be confronted successfully with the use of the Femtosecond Laser.

